Gastrointestinal (GI) disorders are among the most common health concerns globally, affecting millions of people each year. Ranging from mild indigestion to chronic inflammatory diseases, these conditions can significantly impact quality of life when left untreated. As medical science advances, treatment options continue to evolve—offering improved symptom relief, long-term disease management, and better overall digestive health. Understanding the fundamentals of treating GI disorders is an important step toward recognizing symptoms early, seeking proper care, and adopting habits that support a healthy digestive system.
Understanding GI Disorders
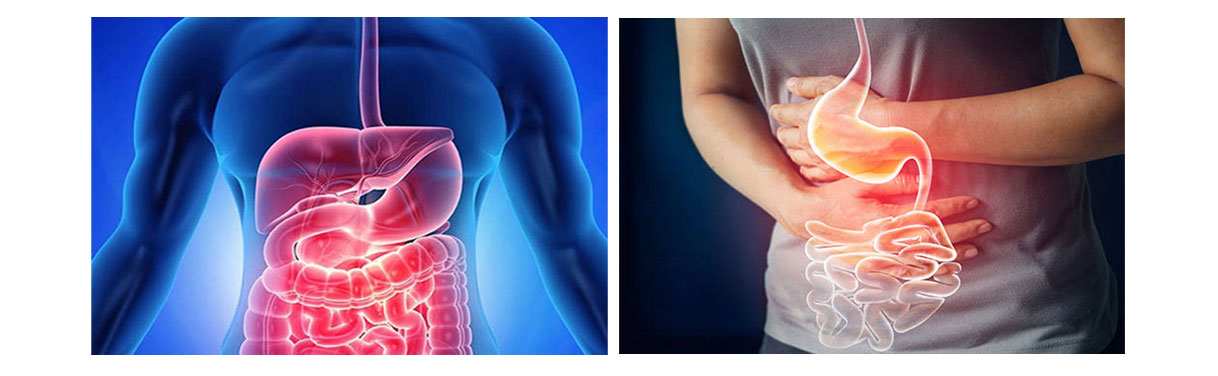
The gastrointestinal system stretches from the mouth to the anus and includes organs such as the esophagus, stomach, intestines, liver, pancreas, and gallbladder. Because it plays a vital role in digestion, absorption, and waste elimination, any disruption in this system can lead to discomfort and dysfunction.
Common GI disorders include:
- Acid reflux and GERD (Gastroesophageal Reflux Disease)
- Irritable Bowel Syndrome (IBS)
- Inflammatory Bowel Disease (Crohn’s disease and Ulcerative Colitis)
- Gastritis and peptic ulcers
- Constipation and diarrhea
- Lactose and gluten intolerance
- Gallstones and pancreatitis
Each disorder has its own underlying causes, ranging from lifestyle factors and dietary habits to infections, immune dysfunction, and genetic predisposition.
Diagnosis: The First Step in Proper Treatment
Effective treatment begins with a clear and accurate diagnosis. Health professionals may use a combination of:
- Medical history and symptom review
- Physical examination
- Blood and stool tests
- Endoscopy or colonoscopy
- Imaging tests such as ultrasound, CT, or MRI
- Breath tests for detecting bacterial overgrowth or lactose intolerance
Proper diagnosis is crucial because digestive disorders often share overlapping symptoms. A tailored treatment plan ensures that patients receive therapies that address the underlying problem rather than only masking symptoms.
Lifestyle and Dietary Modifications
For many GI disorders, especially mild to moderate ones, lifestyle changes can be highly effective. These modifications often form the foundation of treatment, even when medications or procedures are required.
1. Diet Adjustments
Diet plays a significant role in digestive health. Recommendations may include:
- Reducing spicy, acidic, or fatty foods for individuals with acid reflux
- Increasing fiber intake to help with constipation
- Following a low-FODMAP diet for IBS sufferers
- Avoiding trigger foods such as dairy for those with lactose intolerance
Keeping a food diary helps track patterns and identifies sensitivities.
2. Hydration
Adequate water intake supports digestion, prevents constipation, and helps maintain the proper functioning of the GI tract.
3. Regular Physical Activity
Exercise encourages bowel movement regularity, reduces stress, and helps regulate metabolism—all beneficial for digestive health.
4. Stress Management
Since the gut and brain are closely connected, practices like meditation, yoga, and mindful breathing can significantly improve symptoms—especially in conditions like IBS.
Medications and Pharmacological Therapies
Depending on the diagnosis, medical professionals may recommend specific medications, such as:
- Antacids, H2 blockers, or proton pump inhibitors (PPIs) for acid reflux and GERD
- Antispasmodics for abdominal cramps associated with IBS
- Laxatives or stool softeners for chronic constipation
- Antidiarrheal medications to control frequent loose stools
- Antibiotics for bacterial infections, such as H. pylori
- Anti-inflammatory drugs or immunomodulators for inflammatory bowel diseases
- Enzyme supplements for pancreatic insufficiency or lactose intolerance
Medications should always be taken under medical supervision to prevent side effects or drug interactions.
Advanced and Procedural Treatments
For more serious or persistent GI disorders, additional procedures may be necessary, including:
- Endoscopic treatments for bleeding ulcers or removing polyps
- Gallbladder removal surgery for recurrent gallstones
- Bowel resection surgery for severe Crohn’s disease or obstructive conditions
- Minimally invasive procedures for reflux management in certain cases
Modern medical technologies have made many of these procedures safer, quicker, and more effective.
The Importance of Ongoing Care
GI disorders, especially chronic ones, often require long-term management. Regular follow-ups ensure that treatments remain effective and help prevent complications. Patients with conditions like IBD or chronic gastritis benefit from periodic monitoring to track inflammation levels and adjust therapies as needed.
Preventive care is equally important. Routine checkups, early screening procedures (such as colonoscopies), and awareness of family medical history can greatly reduce the risks of serious GI conditions.
A Holistic Path to Digestive Wellness
Treating GI disorders is not about a one-size-fits-all approach—it involves a combination of medical care, healthy lifestyle habits, and continuous awareness of one’s body. With timely action, proper guidance, and a commitment to digestive health, most GI conditions can be effectively managed, allowing individuals to live full, energetic, and comfortable lives. If you experience persistent or severe digestive symptoms, consult a qualified healthcare professional for personalized evaluation and care.